Build Effective Social and Behavior Change Strategies


The Philippines met the coronavirus pandemic with some of the strictest and earliest lockdown measures in Asia, yet cases continue to grow. In fact, as of April 21, 2020, the Philippines has the highest number of coronavirus infections in South and Southeast Asia. Complicating the crisis is the country’s ongoing struggle with tuberculosis – they have the third highest rate of TB in the world. Up to this point, cases and deaths have been concentrated in urban areas in and around Manila, though epidemiologists fear that the disease could spread to rural areas outside the city.
For greater situational awareness, we did a point-of-interest (POI) analysis based on COVID risk factor indicators. Our team looked at communities to the north and south of Manila within 5 kilometers of a hospital. The findings reveal that regional and even provincial level statistics belie significant variations between hospitals and their immediate communities in the Philippines. To more accurately assess the conditions on the ground, our team used machine learning models to quantify important differences that could guide response strategies.
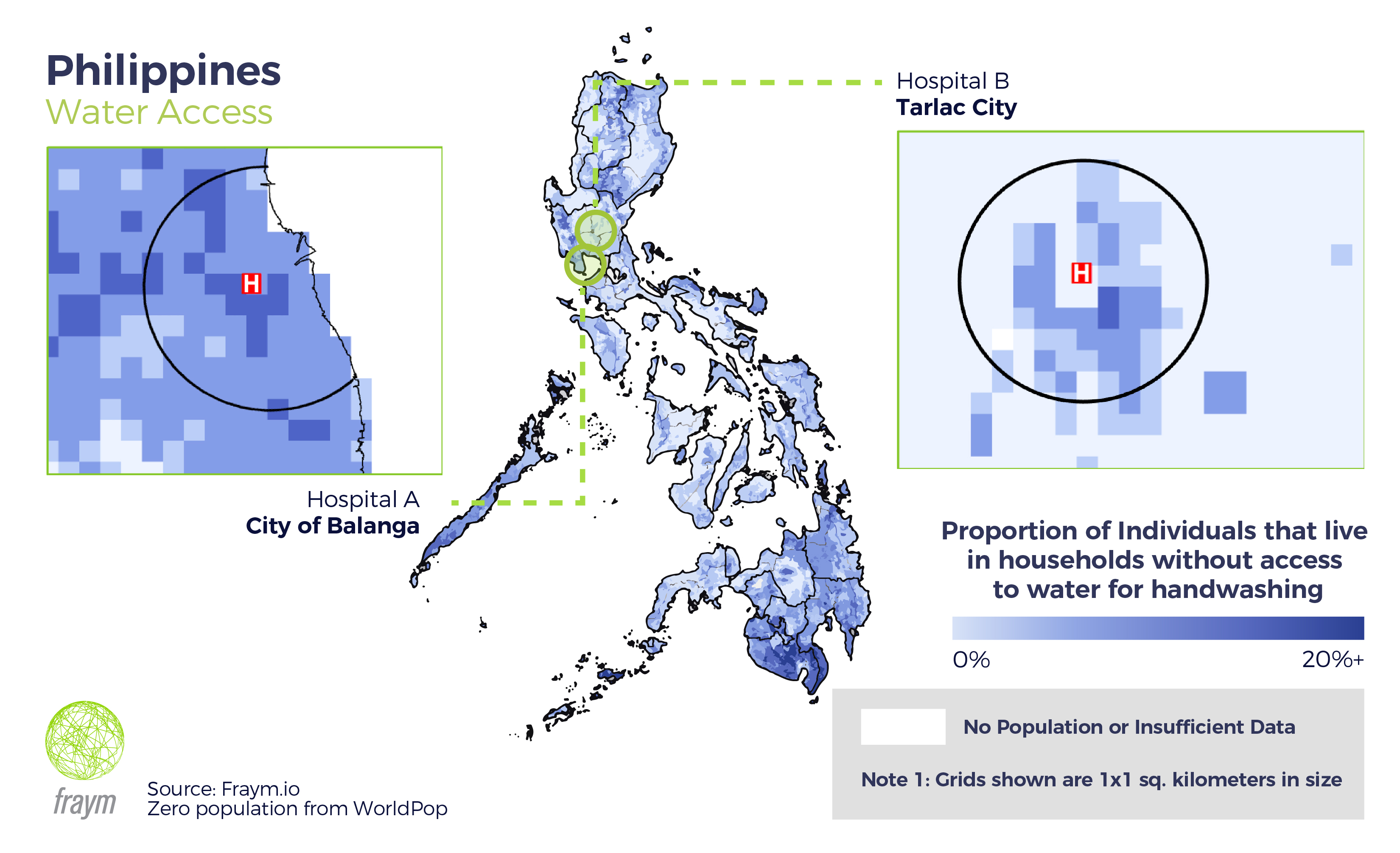
For example, in the same northern region of Central Luzon, two hospitals face different challenges to mitigating COVID 19. The first in the city of Balanga serves a community with more households without access to water for handwashing than the regional average, and a highly mobile population with almost half (48%) owning a scooter. However, for a hospital in Tarlac City to the northeast, only 6% lack access to water for handwashing, though the community has a similar level of scooter ownership. Within the same region, different hospitals face different potentials for the severity of the pandemic.
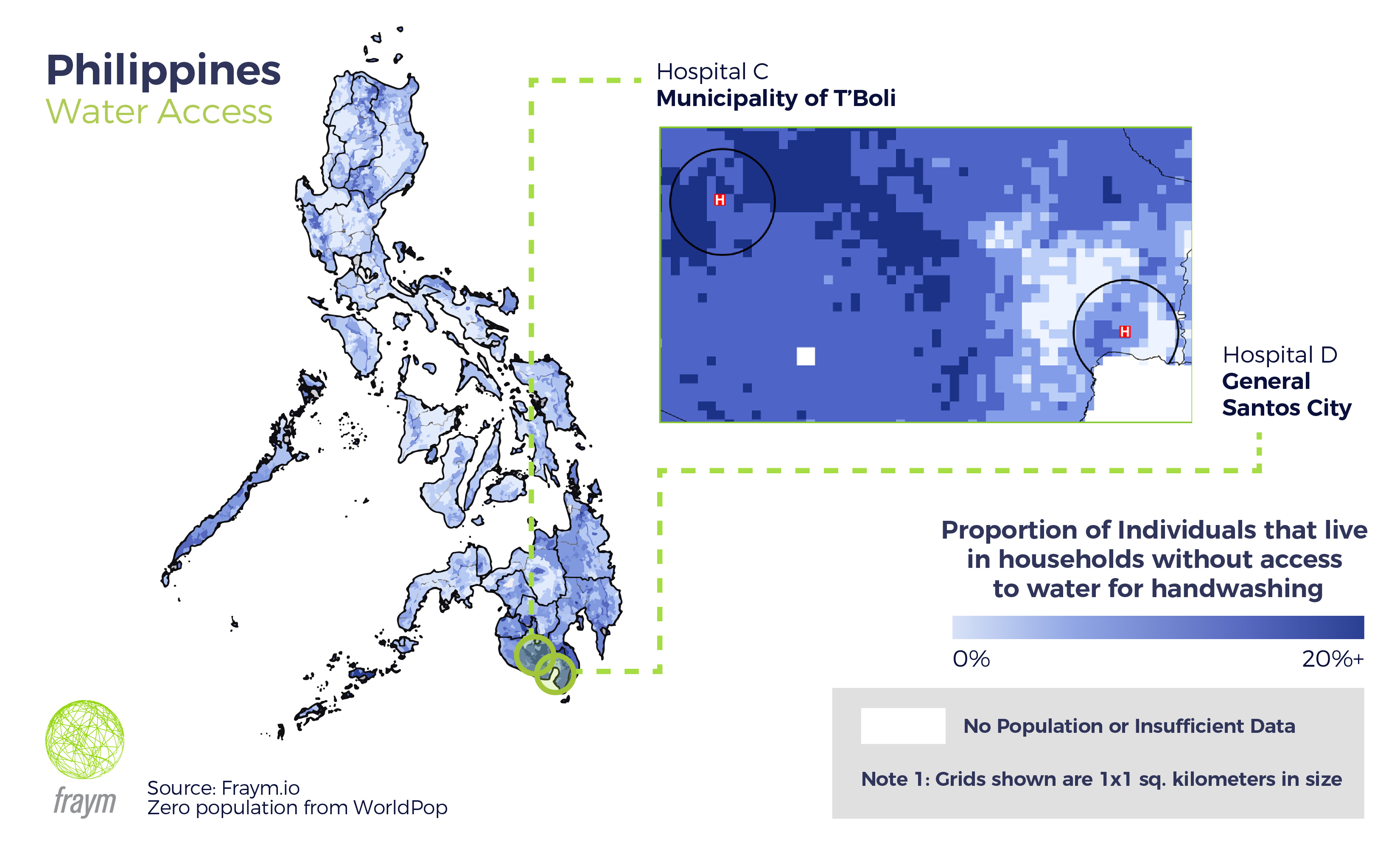
Communities in the southern region of Soccsksargen are similarly varied, even those within the same province. Adding on data for smoking as a risk factor to COVID 19 morbidity highlights even greater challenges for the two hospitals. Within 5 kilometers of a hospital in General Santos City, 8% of individuals do not have access to water for handwashing, a third live in households with a regular smoker, and 14% own a car. Moving to the west still within South Cotabato province, the local hospital in T’Boli serves a far less wealthy and more susceptible population, with only 4% owning a car, 30% without access to water for handwashing, and nearly half (46%) of individuals living in a household with a regular smoker.
Community attributes vary from neighborhood to neighborhood, and during a public health crisis, an awareness of these differences can contribute to the efficacy of response plans. Within a single region, health facilities may be serving vastly different communities with varying levels of resources like clean water and soap. Using specially designed algorithms, like those built by Fraym, governments and organizations can develop targeted interventions that bolster health facilities across the Philippines and the global south.