Mapping Populations for Vaccine Equity

Fraym technology mapped communities across Ethiopia to better understand who is most at-risk to TB, their access to health services, and the most effective communication channels to reach them.
Tuberculosis (TB) remains the third leading cause of death among communicable, maternal, neonatal, and nutritional diseases in Ethiopia, despite being preventable and treatable.1 While Ethiopia continues to make steady progress towards eliminating TB within its borders, lack of access to early diagnosis, treatment and HIV co-infections continue to pose significant challenges.
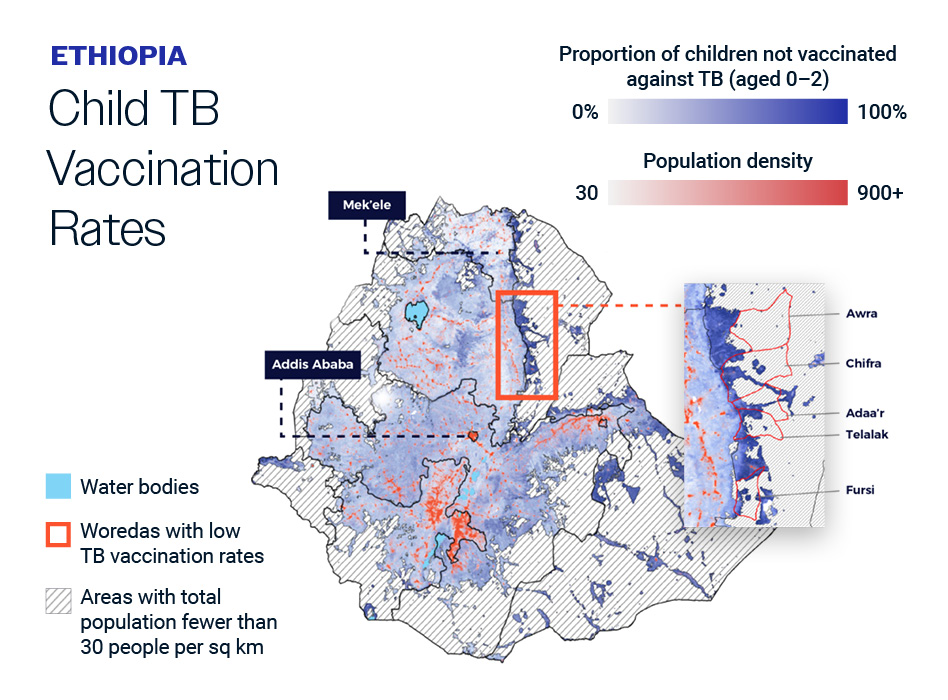
Analysis shows that this at-risk group is largely concentrated in rural, pastoralist communities with low population density.
Nationally, 49% of children under-2 in Ethiopia are unvaccinated against TB – in the Afar region the average is 68%. he five woredas with the lowest vaccination rates in the country are all within Afar: Fursi, Awra, Adaa’r, Telalak, and Chifre – with 76% to 81% of children under-2 unvaccinated against TB.
Within the Afar region, 32% of individuals are under-nourished – nearly ten percentage points above the national average – which increases the risk of infection and severity of tuberculosis.
Moving beyond health metrics, Fraym’s demographic, socioeconomic, and health facility data provides a more holistic understanding of these woredas. For example, communities within the Afar region are significantly more socioeconomically vulnerable than the national average across a number of indicators such as employment, asset ownership, housing, and other community-level data.
This type of TB is difficult to diagnose without more advanced diagnostic tools such as molecular testing and is resistant to the first-line treatment medication Pyrazinamide. As a result, infections are often misdiagnosed and subsequently not treated properly. Pairing this health, facility, socioeconomic, and cultural data together is critical in designing tailored and effective health service delivery interventions that reach the most vulnerable populations.
Fraym started by using ML-derived data to map unvaccinated children across the country.
The national averages mask significant spatial differences and some communities may see only 1 in 5 children vaccinated.
Understand the underlying factors affecting vaccination rates.
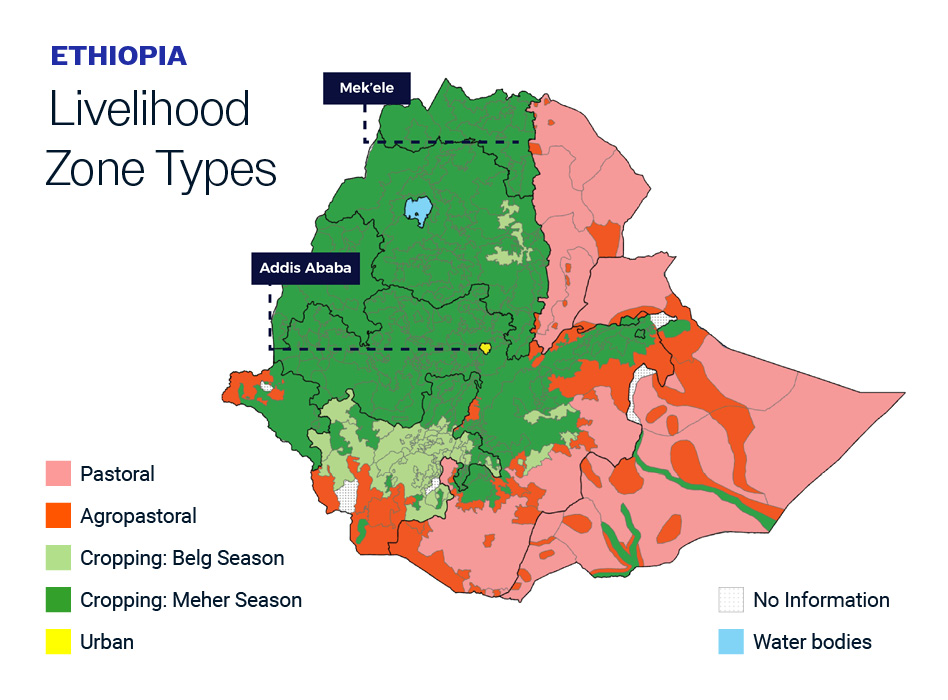
Pastoralism is the prevailing livelihood in the region raising the risk of zoonotic transmission of mycobacterium bovis (bovine TB) from cattle.
/5
Vaccinated in Some Rural Communities
/5
Limited Health Access Score
%
of households have no Internet, Radio, or TV
Finally, Fraym’s communications consumption data highlights how non-traditional messaging may be critical to reaching pastoralist communities in Afar for Social Behavior Change (SBC) interventions. Compared to 57% nationally, 65% of people in Afar live in a household with no radio, no television, no internet access, and no adult in their household who regularly consumes media through the radio, television, or newspaper.5 Mobile phone ownership, however, is comparable in Afar to national levels, at 57% compared to 60%. Given this information, traditional media campaigns may fail to reach some of the most vulnerable households, while a mobile phone campaign is a strong alternative. Public health stakeholders should explore alternative options, such as theater, sports clubs, or religious gatherings, to boost awareness of and reduce misinformation surrounding TB vaccination, symptoms, and treatment options.
Comprehensive hyperlocal information on communities at risk to TB infection can ensure health programming is more targeted, efficient, and effective. With community-level understanding of TB vulnerabilities and geospatial visualization of this data, Fraym partners can pinpoint and quantify communities most at-risk and tailor health interventions to the unique challenges and resources of those neighborhoods. While TB remains a significant threat to Ethiopia’s most vulnerable, community-level interventions that address local risk factors, access to healthcare, and communications access will contribute significantly to the elimination of this disease. Community-level data is an essential tool for achieving a TB-free Ethiopia.